Mamta Bhushan Singh, MD, and Michael F. Finkel, MD

Mamta Bhushan Singh, MD
The medical world thinks of the developed and developing societies in terms of diagnostic and treatment differences. However, there are realities that are common to both spheres concerning most medical conditions.
As a medical student, one would read of common disorders that were not being treated. Epilepsy was a striking example. In many rural Indian communities, up to 90 epilepsy patients out of every 100 were not getting treatment. In bureaucratese, this was a treatment gap of 90 percent.

Michael F. Finkel, MD
The treatment of epilepsy has since evolved. Over two-dozen antiepileptic drugs are currently available. Many drugs are off patent and generically manufactured, and available in India and other developing nations at reasonable prices. But the epilepsy treatment gap of up to 90 percent still exists in many rural Indian communities! So, why has nothing changed for the lot of millions of epilepsy patients?
Let us humanize the numbers. By using calculations from an often-quoted epilepsy prevalence figure of 1 percent of the population, at least 12 million Indians are struggling with epilepsy.1 Large prevalence studies are unavailable, and many experts agree that this number is more likely to be closer to 15 million or even higher. This implies that more than 10 million epilepsy patients in India are untreated. Extrapolating worldwide, there are more than 50 million epilepsy patients and at least 40 million of these reside in developing countries. The estimate is that 75 percent of patients in developing countries are outside the domain of any kind of effective treatment. This implies at least 30 million untreated persons.
Ironically, epilepsy is one of the relatively easily controllable neurological diseases.
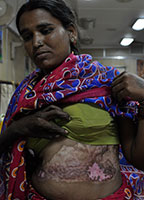
Untreated epilepsy with frequent generalized tonic-clonic seizures results in serious injuries and burns. Patients may lose sight, digits, or limb. The visible scars are further stigmatizing for patients who struggle with societal acceptance. Photo credit: Priya Jain.
What is life like with untreated epilepsy? Most persons with epilepsy who do not have any other neurological illness are essentially normal at all times other than during their seizures. A seizure generally lasts for a few minutes during which, amongst other things, the person is unaware of his or her surroundings, and after which the person may remain confused for a variable amount of time or may sleep off the effects. In either case, the individual is back to normal within a few hours, often without even requiring a trip to the doctor’s clinic or the emergency room.
Then what is the great problem about having untreated active epilepsy with an occasional seizure? Imagine having brief episodes of unawareness just once or twice in a month, in six months or even in a year, but not knowing when these would happen. So, you may be driving to work, crossing the street, climbing a tree, in bed with your partner, swimming in the pool, or speaking mid-sentence in that all important meeting. Suddenly, out of the blue, you start convulsing or just fidgeting with your buttons or speaking in an unintelligible jargon or wet your clothes in full public gaze. How would it feel to know that you had done either of these, and then have to go back to the same people in front of whom this had happened? Well, that is assuming that these people agree to work or socialize with you after witnessing a seizure.
The economic impact of untreated epilepsy is formidable in all societies. Many untreated epilepsy patients remain unemployable, especially if local attitudes consider it to be a contagious disease, a mental illness, or a demonic possession. Thus, they are removed as contributors to the economy. Even if they are poor and have minimum wage jobs, this still adds up to a substantial amount of money loss because of the millions affected.
There are other grave consequences of untreated epilepsy. If the patient is of school or college age, they are very likely to have to drop out. This is either due to their parents’ fear that their child may be injured during a seizure, or on the insistence of teachers. With limited scope for education, landing a good job later in life is subsequently reduced. The intrigue and misinformation surrounding epilepsy reduces social acceptance of patients. Any relationship, including a stable marriage, especially for women with epilepsy, is unlikely. Abandonment of women with epilepsy and their children from marital relationships is common. Such women, with little or no education, no skills and sometimes also with small children to take care of, are often left at the mercy of an impoverished community.
So, is epilepsy difficult to treat? No. Epilepsy is a relatively easy disease to treat in most patients. The diagnosis is clinical and based upon eliciting a history of stereotyped episodes during which the patient may behave abnormally, have involuntary movements or jerks, generally become unaware of his surroundings and then recover in a short time. After the clinical diagnosis, a couple of investigations— EEG and brain imaging — may be done. Investigations may help in deciding the best anti-epileptic drug, in prognosticating how long the treatment is likely to be needed, and how responsive to treatment the patient’s epilepsy might be.
However, even if investigations are not available, as is the case in many developing countries, most patients can still be started on treatment based on clinical history and examination alone. Treatment costs are not very high with generic medications. For example, in India, patients who are treated with one antiepileptic drug spend about $2-$5 per month. Many other developing countries face severe shortages of antiepileptic medication and also have to contend with high medication costs. Along with starting antiepileptic drugs, it is necessary to educate and inform patients at the first visit and at every subsequent opportunity, about their disease and it’s treatment. Without backing up drug treatment with education or “epilepsy literacy,” outcomes are unlikely to be good. After starting treatment, regular reviews at least once or twice a year are needed. Patients have to continue treatment for several years. At least 60-70 percent of epilepsy patients will become seizure-free on medication quite easily. The remaining minority have more difficult forms of epilepsy and need further evaluation and treatment at a specialized epilepsy center. Surgery may be an option for some of these difficult patients.
What are the main challenges? Despite the relative simplicity of the process of epilepsy diagnosis and initiating treatment, millions remain untreated in India and the developing world. To our minds, the biggest hurdles are reliance on specialist doctors who are either entirely missing or extremely scarce and located only in a few large metropolitan cities. This produces a lack of organized, credible, and easily accessible primary care throughout these countries.
Hence, we have the current situation in these countries, where effective systems are not in place. For example, even if an epilepsy patient in a rural area is aware that visiting a doctor and getting the condition treated is possible, what can he do? To whom does he or she go? There is no easy track for one to follow. In India, a hierarchy of health centers exists with a scaling up in staff skill and numbers, and improvement in facilities based upon the size of the population being served. However, doctors and services are not reliably available at these facilities. As a result, an epilepsy patient in a village can either spend an entire lifetime untreated and seizing, or, if he or she is feisty, may make a long and expensive journey to a big city for treatment. No patient should have to do that. In India, there are about 638,000 villages with difficult access. Therein lies the problem. Unless treatment is made available within a radius of about 25-50 kilometers of every small village and town, epilepsy patients and the nation’s economy will continue to suffer needlessly.
Some epilepsy is also preventable. Millions of epilepsy patients in India and worldwide have what is best described as “preventable epilepsy.” In other words, their epilepsy should not have even happened in the first place. Tapeworms cause epilepsy associated with neurocysticercosis. It reflects lack of access to clean food and water, poor sanitation and hygiene, and is an illustration of the public health aspect of epilepsy. Accidents, including frequent road traffic accidents, may lead to head injury and posttraumatic epilepsy. This form of epilepsy is notoriously difficult to treat and often requires surgery. Birth injuries and hypoxic brain damage are more likely to occur with unsupervised childbirth at home. This practice is diminishing, but still prevalent in many rural communities in the developing world. Such babies may also have epilepsy in addition to cerebral palsy, mental subnormality, and behavioral abnormalities. Other preventable epilepsies include epilepsy associated with other brain infections, and drug and alcohol abuse.
How can we overcome epilepsy? Clearly, what the medical community and governments have been doing so far has not worked. The International League Against Epilepsy celebrated its centenary in 2009. The WHO has existed for seven decades. Work has definitely been done and some progress made. But it is too little and at a very slow pace. Times have changed, and many newer resources are available. The need of the hour is a paradigm shift in all aspects of epilepsy care.
We need to think about who will shoulder the responsibility of caring for epilepsy patients in communities where there is a shortage of doctors and specialists. Can the epilepsy care workforce be expanded beyond doctors? Can epilepsy only be diagnosed by seating the patient in front of a doctor in a hospital clinic setting, or are there other viable, safe, and acceptable options? Do patients have to be transported to big city hospitals for investigations or can this also be done in heretofore-overlooked settings?2 Once started on treatment, can regular patient reviews only be done in clinics, or can they be done remotely by telemedicine? Untreated epilepsy can no longer be considered just another medical condition. It is a public health issue. Lives are being impacted as adults become unemployable and the caretaker is likewise reduced in their workforce role.
If diagnosing and treating epilepsy remains only an epileptologist’s, neurologist’s, or even a general physician’s brief, then in developing countries like India, untreated epilepsy will never go away. Non-specialists such as paramedical personnel, district health workers, and nurse clinicians need to be trained and enlisted to expand the epilepsy workforce. Technology is now becoming available for various aspects of epilepsy care and can be pressed into action. Evidence is accruing that epilepsy diagnosis by non-physicians using a phone application is possible.3 This can at least be used as a screening tool in remote rural communities. Nurse-led epilepsy clinics may be considered.4 Diagnosing and starting treatment using mobile rural outreach clinics and patient follow-up using the ubiquitous mobile phone are all viable options that hold promise.5,6
Finally, unless efforts at diagnosing and starting treatment are not accompanied by concerted efforts of raising epilepsy literacy amongst patients, caregivers, and laypersons, success will remain elusive. An Epilepsy Resolution approved by the World Health Assembly on the May 26, 2015 is considered a historical landmark. This resolution was overdue and now societies need to push hard to make it work.
Are countries really too poor to bargain for generic drugs for their citizens? The defense budget of India for 2015-16 is $40 billion, and even a 1 percent reduction in this may be enough to treat the currently untreated epilepsy patients for one year. Reducing the country’s nuclear spend marginally or even getting a sliver of funds spent by the Board of Cricket Control in India may be enough for funding epilepsy treatment in untreated patients. Savings can be achieved in developed countries by allowing the treating personnel to use the appropriate generics rather than the cheapest ones, a common conundrum for U.S. physicians, since the cheapest are not always the most effective. This promotes more seizures and more expenses related to caring for the additional seizures and related injuries. A statement has been attributed to former Secretary of State Condoleezza Rice that the U.S. budget for military bands is higher than that for the U.S. State Department. Certainly these funds can be diverted to effective treatments for uninsured U.S. citizens, rather than to ceremony. Even where universal health care exists, there are expenses that can be cut to fund these physician-prescribed needed medications.
References
- www.who.int/mediacentre/factsheets/fs999/en/
- www.bostonglobe.com/business/2015/05/21/mobile-health-technology-helps-tackle-epilepsy bhutan/c6vmO7XOznyDegIa4BYSAM/story.html
- Patterson V. Singh M. Rajbhandari H. Vishnubhatla S. Validation of a phone app for epilepsy diagnosis in India and Nepal. Seizure 30, 2015, 46–49
- Paul P. Agarwal M. Bhatia R. Vishnubhatla S. Singh MB: Nurse-led epilepsy follow-up clinic in India: is it feasible and acceptable to patients? A pilot study. Seizure; 2014;23(1): 74-6
- Bigelow J. Singh V. Singh M. Medication adherence in patients with epilepsy after a single neurologist visit in rural India. Epilepsy Behav. 2013 Nov;29(2):412-5
Mamta Bhushan Singh, MD, DM is an additional professor, department of neurology, All India Institute of Medical Sciences, New Delhi, India.
Michael Finkel is a retired neurologist, and a member of the AAN, Child Neurology Society, ENS, EFNS, and BMA. He is a fellow of the AAN.
