By Avindra Nath, MD, and James Sejvar, MD

James Sejvar, MD

Avindra Nath, MD
In recent years, there has been an emergence of several major viral infections with devastating neurological consequences, including West Nile virus, dengue, chikungunya, enterovirus D68, Ebola and now Zika virus. Increased global travel and climate change, leading to changing patterns of vector distribution and behavior are among the major reasons for the emergence of these infections. Zika virus is the most recent epidemic that is having devastating effects on human populations in affected regions, and is rapidly spreading across the South American continent.
Epidemiology
Zika virus was first identified from a primate in 1947 in the Zika forest of Uganda.1 The first human cases occurred in Africa and then in Southeast Asia in the 1960s.2,3 During the intervening years, Zika virus was associated with isolated cases or small outbreaks mainly in Africa. In 2007, there was an outbreak in Yap, the Federated States of Micronesia, where nearly three-quarters of the population was infected.4, 5 This represented the largest outbreak of Zika virus infection to that point. In 2013, there was an epidemic in French Polynesia, which was associated with a reported increase in cases of the autoimmune peripheral nerve disorder Guillain-Barre syndrome, although a causal association between Zika virus and Guillain-Barre syndrome was never established.
In December 2014, Zika virus was first detected in Brazil. Although it is unknown how it was introduced into Brazil, some hypothesize that a traveler attending the 2014 football/soccer World Cup introduced the virus. The outbreak in Brazil was fast moving and large. Tens of thousands of people became ill, and likely millions of people were infected. Similar to French Polynesia, shortly after the beginning of the Zika virus outbreak, clinicians began reporting larger-than-expected numbers of Guillain-Barre syndrome. Many of these people had reported a febrile rash illness compatible with Zika in the days or weeks before their weakness onset. In addition, clinicians in Brazil noted a 20-fold increase in microcephaly in 2015, compared to previous years, with microcephalic babies born approximately eight to nine months after the first recognition of Zika virus. Some of the infants’ mothers reported a rash illness compatible with Zika virus infection while pregnant, leading to the suspicion that the microcephaly was somehow associated with Zika virus infection.
Nearly 90 percent of the cases of microcephaly occurred in the northeastern region of the country,6, 7 areas experiencing some of the heaviest burdens of Zika virus infection as well. French Polynesian health authorities reported an unusual increase in central nervous system malformations in babies born during a Zika virus outbreak on the islands from 2014 to 2015.6 The infection has now spread across most of South America and Mexico. To date, few cases have been reported in the United States among travelers returning from Zika virus-affected regions.8, 9
Virology and Pathophysiology
Zika virus is a positive-sense, single-stranded RNA virus (genome 10.7 K nucleotides) belonging to the flaviviridae family, which includes dengue, yellow fever, Japanese encephalitis, St. Louis encephalitis and West Nile virus. It has the ability to cross the placenta and cause developmental brain abnormalities in children, suggesting that the virus likely infects neural stem cells. The severity of brain malformations may be related to the stage of fetal development at the time of infection. Microcephaly would be the most common manifestation, but if infection were to occur in earlier stages of fetal development, anencephaly or lissencephaly may occur.
The pathophysiology of ascending paralysis and myelitis in adults is unknown. However, mice injected with the virus can develop paralysis, suggesting direct invasion by the virus, although an immune-mediated, post-viral syndrome is also possible. It remains unknown if once infected and recovered if an individual develops long-term immunity or not, and if recurrent infections or relapses can occur. Questions regarding long-term viral persistence in tissue reservoirs also remain unanswered.
Transmission
The virus is transmitted by the Aedes species of mosquitoes 10, in particular Aedes aegypti, the vector involved with transmission of dengue, a closely related flavivirus. Additionally, experimental evidence suggests the virus can be transmitted by Asian tiger mosquitoes (Aedes albopictus) 11, 12, which can survive in cold temperatures. Most arboviruses have an intermediary host or “reservoir.” For West Nile virus, birds, particularly corvids, serve as these reservoirs. For Venezuelan, Western and Eastern equine encephalitis viruses, horses serve this role, and for Japanese encephalitis virus, it is primarily pigs. However, the transmission of Zika virus generally occurs directly between humans and mosquitos. There is some evidence that human-to-human transmission may occur through sexual intercourse, and the virus has also been detected in saliva, so the potential for oral transmission also exists. The virus has been isolated from the amniotic fluid of pregnant women and blood and tissues of newborns, suggesting materno-fetal transmission.13 So far, an intermediary host has not been identified.
Clinical Manifestations
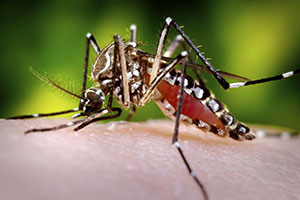
Female Aedes aegypti mosquito
The majority of Zika virus infections — 80 percent — are clinically asymptomatic.4 Among persons who develop symptoms, Zika virus infection is generally considered to be mild, causing fever, rash and body aches. Some may develop conjunctivitis. Symptoms usually last one week.
The full spectrum of neurological complications from this viral infection remains unknown. The epidemiological association between microcephaly and the infection seems strong. In Brazil, annual reported rates of microcephaly would generally be somewhere around 150 cases per year. Reportedly, between October 2015 and January 2016, more than 3,500 babies were born with the condition. CT brain scans show evidence of widespread calcification. Other malformations, such as anencephaly and lissencephaly, might also occur. It remains uncertain if other organs may be involved in addition to the brain. However, the differential diagnosis of microcephaly is broad. Hence, when presented with a patient with microcephaly, it remains important to consider other common causes, such as genetic, craniostenosis, and infections, such as toxoplasmosis, rubella, varicella zoster virus and cytomegalovirus. Intrauterine cerebral anoxia, exposure to drugs, alcohol and other toxins, malnutrition and metabolic disorders such as phenylketonuria can also cause microcephaly. Patients with microcephaly often have developmental delay, difficulty with gait and balance, mental retardation, seizures and hyperactivity.
Guillain-Barre syndrome appears to be a recurring possible complication of Zika virus infection. Following the introduction of Zika virus into French Polynesia, clinicians began reporting larger-than-expected numbers of Guillain-Barre syndrome cases on the island.14 Following the introduction of Zika virus to Brazil in December 2014, again, reports surfaced of large numbers of Guillain-Barre syndrome cases. In Brazil, few cases of Guillain-Barre syndrome had laboratory confirmation of Zika virus, but currently the primary method of diagnostic testing is through the detection of viral RNA through polymerase chain reaction. In Guillain-Barre syndrome, by the time the clinical features of limb weakness develop, it is unlikely that there would still be circulating virus, and, as such, detection of viral RNA would not be expected. Less commonly, some patients have been thought to have a myelitis or polio-like manifestations. Currently, it is unclear if these are all related or if indeed both spinal cord and peripheral nerves can be involved. Thus, in Brazil, epidemiologic evidence and the close temporo-spatial clustering of both Guillain-Barre syndrome and Zika virus cases provides intriguing circumstantial evidence for an association.
In other cases in which the virus was newly introduced, reported increases of Guillain-Barre syndrome cases have invariably appeared, including in Colombia, Venezuela and, more recently, El Salvador, which reported 46 Guillain-Barre syndrome cases in a five-week period from December 2015 to early January 2016. That is nearly three times more than the country would normally see in that timeframe. Laboratory substantiation of an association between Zika virus and Guillain-Barre syndrome has proved challenging, however. As noted, by the time of onset of weakness, the virus would be expected to be cleared from the body, and molecular techniques to identify the virus or viral RNA would not be expected to be positive. Detection of Zika virus-specific antibodies would provide evidence of current or prior infection. However, that method also has its challenges. Dengue virus is a closely related flavivirus to Zika, and invariably co-circulates in all areas currently associated with Zika virus. However, dengue virus infection has also rarely been associated with Guillain-Barre syndrome, and laboratory testing by serology is challenging due to the substantial cross-reactivity of antibodies between Zika virus and dengue virus.
Since these viruses are carried by the same mosquito vector and co-circulate at the same times of the year, it can be challenging to differentiate between infection with the two viruses.15 Development of a robust serologic assay that can reliably differentiate Zika virus from dengue and other closely related flaviviruses will be crucial in order to provide laboratory evidence of Zika-associated Guillain-Barre syndrome, as well as other late complications of Zika virus. Currently, the nature of the neuropathy is not known, as results of electrodiagnostics to determine the clinical sub-type of Guillain-Barre syndrome possibly associated with Zika virus has been rarely reported. It would be important to know if it is axonal or demyelinating and if it is immune mediated. This could affect treatment and prognosis. Recovery from demyelinating neuropathies is generally better than those due to axonal injury. Isolated reports suggest that the neuropathy may be demyelinating and may respond to treatment with intravenous immunoglobulin.14
Laboratory Diagnosis
Viremia occurs only during the first few days of the illness, but if blood samples are obtained during that time, virus can be detected by polymerase chain reaction.16 Following this phase, IgM antibodies can be demonstrated by ELISA or Western blot analysis. Previous epidemics have noted that there is cross reactivity between antibodies to Zika and other arboviruses such as dengue.5 The Centers for Disease Control and Prevention (CDC) has issued guidelines for the testing of infants born with possible Zika virus infection.17
Treatment and Prevention
Currently, there is no effective treatment or vaccine against the virus. Hence, prevention is key with control of mosquito populations and prevention of mosquito bites. Travel advisories have been issued for pregnant women not to travel to areas experiencing Zika virus outbreaks. For individuals who suffer from the neurological consequences of the infection, long-term supportive and symptomatic treatment is key. The socio-economic impact of the infection, particularly if the association between Zika virus and microcephaly holds true, will likely be huge and felt for decades. While the large number of cases of microcephaly is tragic, whatever the eventual cause turns out to be, it will result in large numbers of children with developmental disorders and begs for the need to train personnel in a wide variety of health disciplines, including neurology, rehabilitation, specialized nursing, social services, etc., to care for and treat this population. Ongoing surveillance for Zika virus in the Americas and elsewhere, to monitor its continued spread, as well as documentation of infection among travelers returning from affected areas will be critical. Development of more robust serologic assays that can differentiate Zika virus from other closely related flaviviruses will be an important tool to substantiate an association between Zika virus and devastating neurologic conditions, such as Guillain-Barre syndrome and microcephaly. Ultimately, the long-term epidemiologic pattern of Zika virus will be important to monitor.
References:
- Weinbren, M.P. and M.C. Williams, Zika virus: further isolations in the Zika area, and some studies on the strains isolated. Trans R Soc Trop Med Hyg, 1958. 52(3): p. 263-8.
- Simpson, D.I., Zika Virus Infection in Man. Trans R Soc Trop Med Hyg, 1964. 58: p. 335-8.
- Olson, J.G., et al., Zika virus, a cause of fever in Central Java, Indonesia. Trans R Soc Trop Med Hyg, 1981. 75(3): p. 389-93.
- Duffy, M.R., et al., Zika virus outbreak on Yap Island, Federated States of Micronesia. N Engl J Med, 2009. 360(24): p. 2536-43.
- Lanciotti, R.S., et al., Genetic and serologic properties of Zika virus associated with an epidemic, Yap State, Micronesia, 2007. Emerg Infect Dis, 2008. 14(8): p. 1232-9.
- Control, E.C.f.D.P.a., Rapid risk assessment: Zika virus epidemic in the Americas: potential association with microcephaly and Guillian Barre syndrome. 10 December 2015.
- Bogoch, II, et al., Anticipating the international spread of Zika virus from Brazil. Lancet, 2016.
- Control, C.f.D., CDC telebriefing: Zika virus travel alert. 15 January 2016.
- Hennessey, M., M. Fischer, and J.E. Staples, Zika Virus Spreads to New Areas – Region of the Americas, May 2015-January 2016. MMWR Morb Mortal Wkly Rep, 2016. 65(3): p. 55-8.
- Li, M.I., et al., Oral susceptibility of Singapore Aedes (Stegomyia) aegypti (Linnaeus) to Zika virus. PLoS Negl Trop Dis, 2012. 6(8): p. e1792.
- Grard, G., et al., Zika virus in Gabon (Central Africa)–2007: a new threat from Aedes albopictus? PLoS Negl Trop Dis, 2014. 8(2): p. e2681.
- Wong, P.S., et al., Aedes (Stegomyia) albopictus (Skuse): a potential vector of Zika virus in Singapore. PLoS Negl Trop Dis, 2013. 7(8): p. e2348.
- Pan American Health Organization and World Health Organization. Epidemiological Alert: Neurological syndrome, congenital malformations, and Zika virus infection. Implications for public health in the Americas. http://www.paho.org, 1 December, 2015.
- Oehler, E., et al., Zika virus infection complicated by Guillain-Barre syndrome–case report, French Polynesia, December 2013. Euro Surveill, 2014. 19(9).
- Carod-Artal, F.J., et al., Neurological complications of dengue virus infection. Lancet Neurol, 2013. 12(9): p. 906-19.
- Faye, O., et al., One-step RT-PCR for detection of Zika virus. J Clin Virol, 2008. 43(1): p. 96-101.
- Staples, J.E., et al., Interim Guidelines for the Evaluation and Testing of Infants with Possible Congenital Zika Virus Infection – United States, 2016. MMWR Morb Mortal Wkly Rep, 2016. 65(3): p. 63-7.
